
Male Fertility Testing 101
Jun 2021Recent Article
Semen Analysis
If you and your partner are struggling with infertility, you are not alone. According to statistics, this significant problem affects 8-12% couples worldwide. Out of these infertility cases, approximately 40–50% can be attributed to male-factor infertility.[1]
To determine the cause and next steps of male infertility, often the first step is through a semen analysis. A semen analysis usually tests 4 parameters:
1. Sperm concentration
Sperm concentration is the measure of the number of sperms per unit volume (millilitre) of sperm. According to the World Health Organisation (WHO), a normal sperm concentration is 15-259 million per millilitre [2]. In natural conception, only a few sperm cells reach the ampulla or the site of fertilisation, so having an adequate amount will help. A study in the journal of Molecular Aspects of Medicine reveals that there’s a positive correlation between Ubiquinol concentration in seminal fluid and sperm count from subjects with a history of infertility.[3]
2. Sperm motility
Sperm motility indicates how sperm move. The movement of sperm impacts whether or not they make it to the egg, and when successful, whether they can penetrate the egg to fertilise it. WHO states 40 – 81% motile sperm to be the normal result [2].
3. Sperm morphology
Sperm morphology refers to what percentage of sperm have the proper shape, size, and structure. When a sperm is deformed, it may have difficulty moving to or fertilising the egg. According to the WHO, a normal morphology result is 4% NF or higher [2].
4. Semen volume
Semen volume is the amount of fluid ejaculated. WHO specifies that a normal semen volume ranges from 1.5ml to 5ml [2]. This can indicate blockage in one or more of the ducts of the male reproductive system and may compound the issue of low sperm count.
A study investigated the effects of the administration of ubiquinol (a reduced form of coenzyme Q10) on semen parameters and seminal plasma antioxidant capacity in infertile men with idiopathic oligoasthenoteratozoospermia. In the study, 228 men with unexplained infertility were randomly assigned 1:1 into 2 groups, group 1 (114) received 200 mg ubiquinol daily by mouth for 26 weeks and group 2 (114) received a similar regimen of placebo. The study found that Ubiquinol was significantly effective in men with unexplained oligoasthenoteratozoospermia for improving sperm density, sperm motility and sperm morphology.[4]
References
[1] Agarwal, A., Mulgund, A., Hamada, A. and Chyatte, M., 2015. A unique view on male infertility around the globe. Reproductive Biology and Endocrinology, 13(1).
[2] WHO laboratory manual for the examination and processing of human semen (2010). 5th edn. Switzerland: World Health Organisation. Available at: http://apps.who.int/. [Accessed 1 June 2021].
[3] Alleva R, Scaramucci A, Mantero F et al. (1997) The protective role of ubiquinol-10 against formation of lipid hydroperoxides in human seminal fluid. Molec Aspects Med 18: s221–s228
[4] Safarinejad, M., Safarinejad, S., Shafiei, N. and Safarinejad, S., 2012. Effects of the Reduced Form of Coenzyme Q 10 (Ubiquinol) on Semen Parameters in Men with Idiopathic Infertility: a Double-Blind, Placebo Controlled, Randomized Study. Journal of Urology, 188(2), pp.526-531.
You can share this by:
Keep up-to-date with Ubiquinol News
Ubiquinol Headlines

Ubiquinol and Healthy Ageing: A Conversation with Dr Denis Furness on the House of Wellness Radio
Jun 2025Category: Ageing, Antioxidants, Broadcast, Energy, Fatigue, Health, healthy ageing, In The News, Mitochondrial health, Ubiquinol, wellnessRead More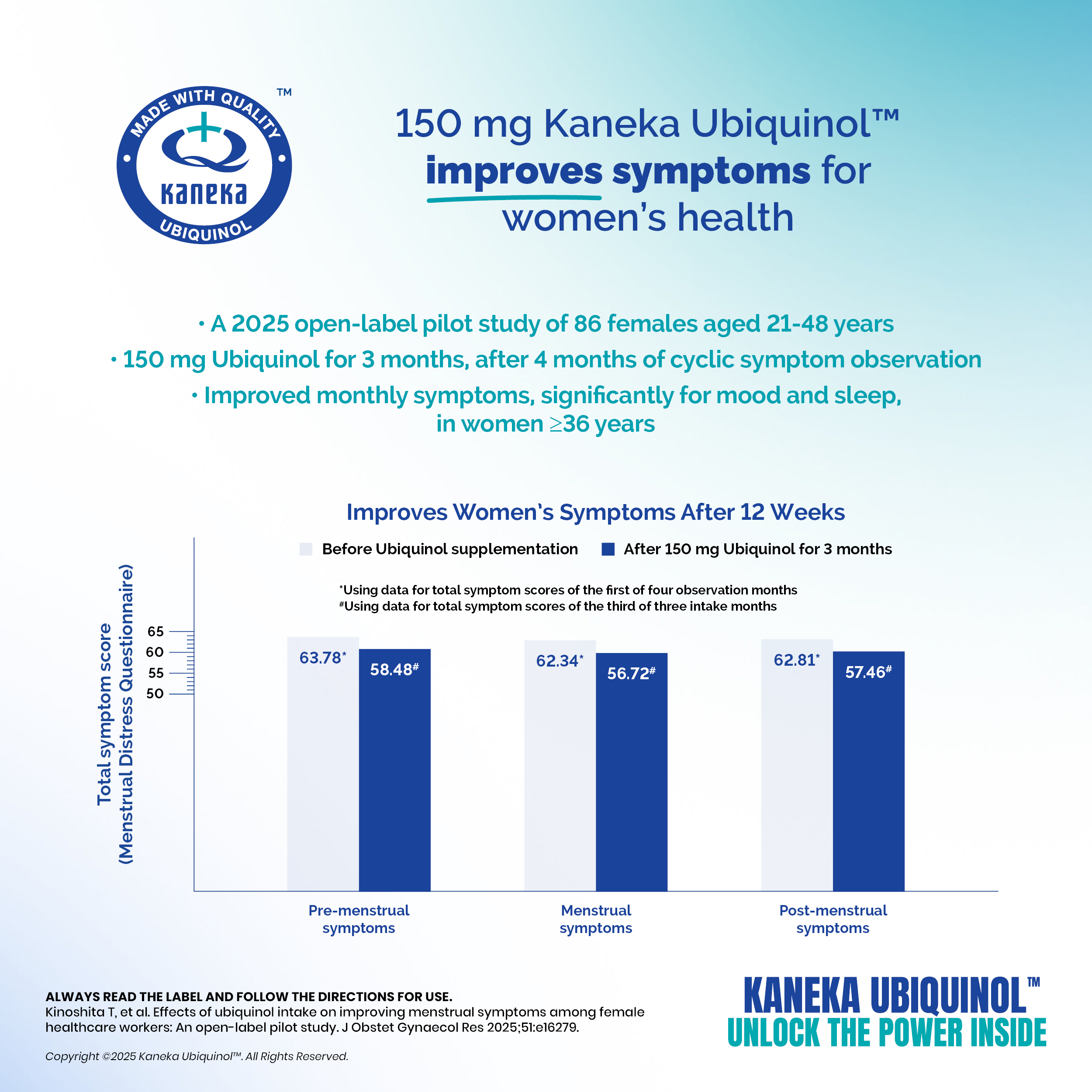
Kaneka Ubiquinol™ for Relief of Women’s Symptoms
May 2025Category: Ageing, Fertility, Menopause, Ubiquinol, wellness, Women's HealthRead More
Mitochondrial Health in Women’s Wellbeing: Key Insights from CMA Innovation Day 2025
May 2025Category: Antioxidants, Conferences, Fertility, Menopause, Ubiquinol, wellness, Women's HealthRead More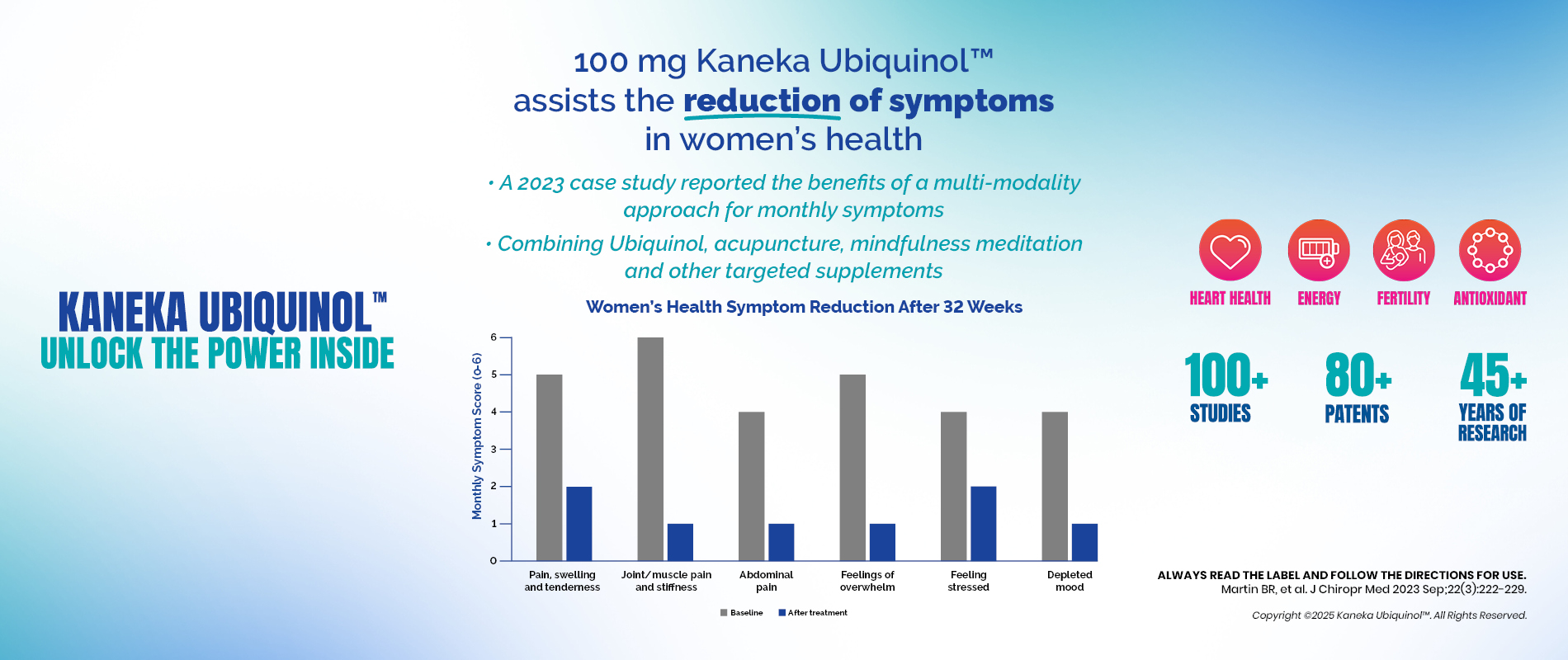
Ubiquinol for Women’s Health
Apr 2025Category: Ageing, Antioxidants, Fertility, Kaneka, Mitochondrial health, Ubiquinol, wellness, Women's HealthRead More
Kaneka Ubiquinol™ at APP 2025: Advancing Healthy Ageing & Longevity
Mar 2025Category: Ageing, Antioxidants, APP, Conference, Conferences, Energy, Fatigue, Health, Health Industry, healthy ageing, Kaneka, Mitochondrial health, Nutrition, UbiquinolRead More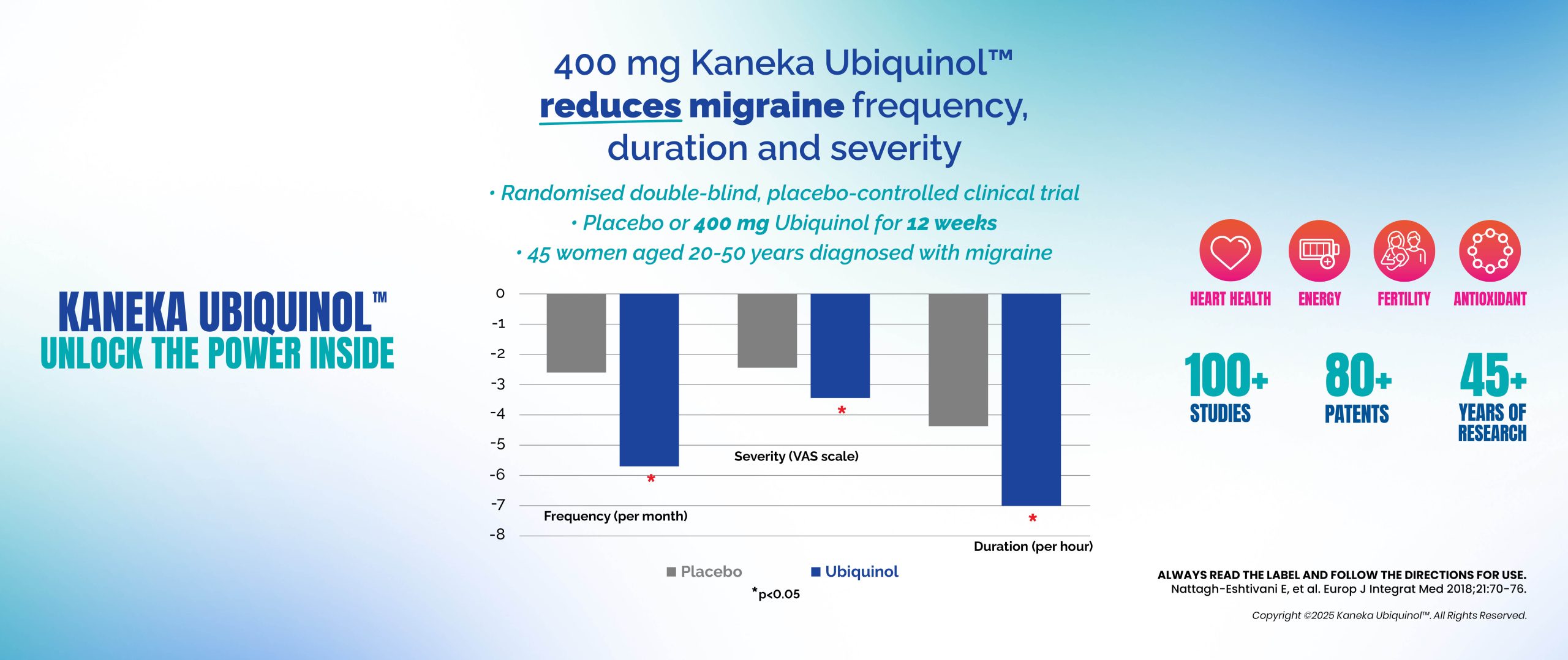
Ubiquinol: Supporting Migraine Relief Through Cellular Energy
Jan 2025Category: Antioxidants, complementary medicine, Energy, Fatigue, Health, Health Industry, healthy ageing, Kaneka, Mitochondrial health, Nutrition, Stress, Ubiquinol, Vitamins, wellnessRead More
Kaneka Ubiquinol™ at Functional Foods for Wellness Industry Awards and Summit, #FFWS2025
Jan 2025Category: Ageing, Antioxidants, Awards, cardiovascular health, Conference, Conferences, Energy, Fatigue, FFWS2025, Health, Health Industry, healthy ageing, Kaneka, Menopause, Mitochondrial health, Nutrition, Ubiquinol, VitaminsRead More




